Available languages:
Table of Content:
What is colorectal cancer?
Colorectal cancer (CRC) is a malignant tumor that forms in the tissues of the colon (the longest part of the large intestine) or of the rectum (the final part of the digestive tract). Colon cancer and rectal cancer are often grouped together because they have many features in common. In EU-27 countries in 2020, colorectal cancer accounted for 12.7% of all new cancer diagnoses and 12.4% of all deaths due to cancer. That made it the second most frequently occurring cancer (after breast cancer) and the second cause of cancer death (after lung cancer).[1]
- Colorectal cancer is the third most diagnosed cancer in men (after prostate and lung cancers) and the second one in women (after breast cancer).
- It is the second cause of cancer death in men (after lung cancer) and the third one in women (after breast and lung cancers).
- Estimated colorectal cancer incidence and mortality rates in 2020 vary two-fold across EU-27.
- The overall colorectal cancer trends are increasing for incidence and decreasing for mortality, but there are national and regional exceptions and large variability among EU-27 countries.
- The five-year survival of colorectal cancer patients diagnosed in 2000-2007 is highest in Western Europe and lowest in some countries of Eastern Europe.
Signs and symptoms of colorectal cancer
Some common signs and symptoms of colorectal cancer include changes in bowel habits, such as diarrhea or constipation, rectal bleeding or blood in the stool, abdominal pain or discomfort, weakness or fatigue, and unexplained weight loss.
However, many people with colorectal cancer do not experience any symptoms in the early stages of the disease.
According to Digestive Cancers Europe[2], colorectal cancer might not cause symptoms right away, but when they do appear, common symptoms may include an ongoing change in bowel habits that lasts for more than a few days (diarrhea, constipation or feeling that the bowel does not empty completely), stools that are narrower than usual, blood (either bright red or very dark) in the stool, rectal bleeding with bright red blood, frequent gas pains, bloating, fullness or abdominal cramps, weight loss for no known reason.
Screening for colorectal cancer
Colorectal cancer screening is a medical test that checks for signs of cancer in the colon and rectum. The purpose of colorectal cancer screening is to detect any potential cancerous growths before any symptoms appear. Getting screened for colorectal cancer is important because it can help detect the disease early, when it is more treatable and curable. Colorectal cancer is one of the most common types of cancer and can develop without causing any symptoms in the early stages. Colorectal cancer screening can help detect the disease before it has a chance to spread to other parts of the body.
Several CRC screening methods are available, each with its own strengths, weaknesses, and effectiveness in detecting cancer or its precursors.[3]
Faecal Occult Blood Testing
The most extensively studied method of CRC screening is faecal occult blood testing (FOBT), which tests for hidden (occult) blood in stool. It’s a non-invasive test that can be done at home and has been shown to reduce CRC mortality by up to 20% if offered biennially and possibly more if offered yearly. This is because the test can detect CRC in the early stages, often before symptoms appear, when treatment is most effective.
Endoscopic screening: sigmoidoscopy and colonoscopy
Endoscopic screening methods like sigmoidoscopy and colonoscopy are more direct ways of detecting adenomas or CRC. These methods use a thin, flexible tube with a light and camera attached to the end to visually examine the rectum and lower or entire colon.
Sigmoidoscopy, which examines only the rectum and lower colon, has been linked to a reduction in distal colorectal cancer incidence in case-control and uncontrolled cohort studies. However, due to a lack of evidence from randomized trials, some countries have been hesitant to introduce sigmoidoscopy as a standard screening method. To address this, ongoing trials in the UK, Italy, and the US are currently evaluating its effectiveness.
Stool DNA testing and virtual colonoscopy
Apart from the traditional methods, researchers are actively investigating new techniques for CRC screening. One promising approach involves extracting DNA from stool samples and testing for specific genetic markers associated with CRC. The sensitivity of these markers for adenomas—precursors to cancer—is not yet fully understood, but early results are promising, showing improved specificity over FOBT.
Virtual colonoscopy, another innovative technique, uses advanced imaging technology to generate a detailed picture of the colon, screening out individuals without neoplasia (abnormal growths) and thus reserving colonoscopy for patients requiring therapeutic intervention. The sensitivity of virtual colonoscopy for large adenomas and CRC appears to be high, making it a potential option for further investigation in patients with positive stool-based screening tests.
EU guidelines recommend average-risk individuals to begin screening for colorectal cancer at age 50 and continue regular screening every 2-10 years depending on the type of test used. People with a family history of colorectal cancer or other risk factors may need to start screening earlier and undergo more frequent testing.
Treatment
If colorectal cancer is found during screening, there are many treatment options available, including surgery, chemotherapy, and radiation therapy. The earlier the cancer is detected, the more likely it is that treatment will be successful, and the person can be cured.
Treatment of colorectal cancer (CRC) has evolved significantly over the years. The complexity of the disease requires a multidisciplinary approach, with a combination of surgery, chemotherapy, radiotherapy, and targeted therapies often needed. The most critical factor in determining treatment strategy is the stage of the disease at diagnosis.[4]
Surgical resection
Surgical resection remains the primary treatment modality for localized CRC, with the goal of removing all tumor tissue and any affected lymph nodes. Technological advancements have led to the development of minimally invasive surgical techniques such as laparoscopic and robotic surgery. These methods have been shown to have comparable oncologic outcomes to conventional open surgery, with the added benefits of reduced blood loss, shorter hospital stays, and quicker return to normal activities. For patients with advanced CRC, neoadjuvant (pre-operative) or adjuvant (post-operative) chemotherapy is typically recommended to reduce the risk of cancer recurrence. Systemic chemotherapy can also play a critical role in managing metastatic disease, potentially shrinking tumors and improving survival.
Targeted therapies
Recent advancements have seen the introduction of targeted therapies that aim to interfere with specific molecular pathways that drive cancer growth and spread. For example, monoclonal antibodies such as bevacizumab and cetuximab target vascular endothelial growth factor (VEGF) and epidermal growth factor receptor (EGFR), respectively, inhibiting tumor growth and progression.
Immunotherapy
In addition to these conventional approaches, immunotherapy has emerged as a promising therapeutic option in certain subsets of CRC patients. Immune checkpoint inhibitors, such as pembrolizumab, have shown effectiveness in patients with mismatch repair-deficient (dMMR) or microsatellite instability-high (MSI-H) tumors.
Personalised medicine and molecular profiling of tumors
Lastly, personalized medicine and molecular profiling of tumors are transforming the management of CRC. By identifying specific genetic mutations in tumors, clinicians can tailor treatment strategies that will be most effective for individual patients.
While significant progress has been made, continued research and clinical trials are crucial to improve treatment strategies and outcomes for patients with CRC. This includes the exploration of novel targeted therapies, optimization of existing treatment protocols, and the ongoing investigation into the genetic and molecular underpinnings of this complex disease.
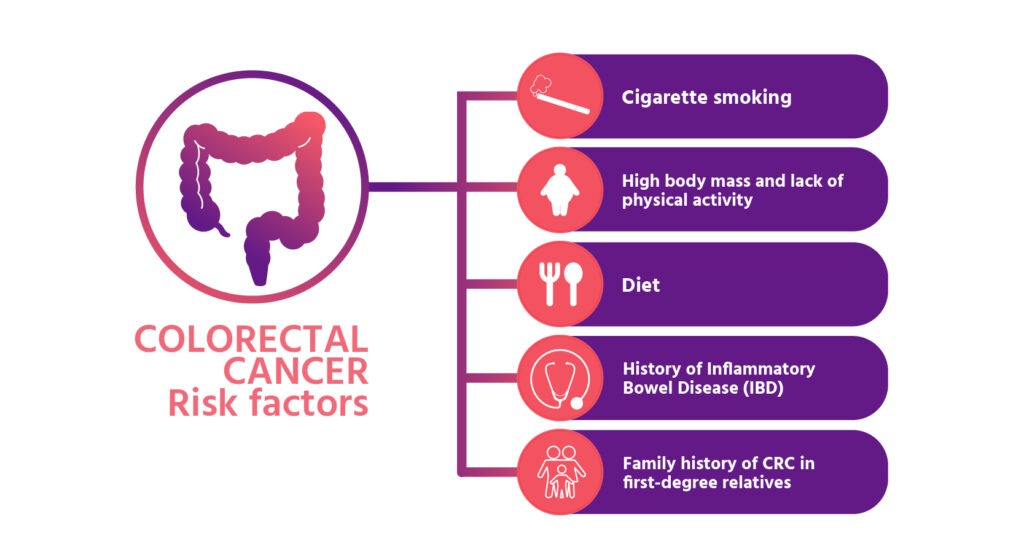
Risk factors
Colorectal cancer (CRC) is a significant health concern worldwide, and understanding the risk factors associated with its development is crucial for prevention and early detection. In a recent scientific article[5], researchers conducted a comprehensive review and meta-analysis to identify and quantify the impact of various risk factors on CRC incidence. By analyzing the published evidence, they shed light on the demographic, behavioral, and environmental factors that contribute to increased risk.
- One of the most striking findings of the study was the association between inflammatory bowel disease (IBD) and CRC. Individuals with IBD were found to have a 2.93 times higher risk of developing CRC compared to those without the condition. This highlights the importance of close monitoring and proactive management of IBD patients to minimize their CRC risk.
- Another notable risk factor is a family history of CRC in first-degree relatives. Individuals with a family history of the disease were found to have a 1.8 times higher risk of developing CRC. This emphasizes the significance of genetic predisposition and the importance of regular screenings and early detection in individuals with a familial history of CRC.
The study also examined the impact of lifestyle factors on CRC risk:
- Body mass index (BMI) was found to be associated with an increased risk of CRC, with a 1.10-fold increase per 8 kg/m² rise in BMI. This highlights the importance of maintaining a healthy weight through regular exercise and a balanced diet to reduce the risk of CRC.
- Physical activity emerged as a protective factor against CRC, with a 0.88-fold decreased risk observed for every two standard deviations increase in physical activity score. Engaging in regular exercise, such as brisk walking or moderate-intensity aerobic activities, can play a role in reducing the risk of CRC.
- Cigarette smoking was found to increase the risk of CRC, with a 1.06-fold higher risk observed for every 5 pack-years of smoking. This underscores the importance of smoking cessation programs and policies to reduce the burden of CRC.
- Dietary factors were also shown to be associated with CRC risk. Consumption of red meat was found to increase the risk of CRC, with a 1.13-fold higher risk observed for every 5 servings per week. On the other hand, higher intake of fruits (3 servings per day) and vegetables (5 servings per day) was associated with a reduced risk of CRC, with risk reductions of 0.85 and 0.86, respectively. These findings highlight the importance of adopting a healthy diet rich in fruits and vegetables while minimizing the consumption of red meat.
[1] Source: ECIS – European Cancer Information System. From https://ecis.jrc.ec.europa.eu, accessed on 19/06/2023 © European Union, 2023
[2] https://digestivecancers.eu/colorectal-symptoms/
[3] W. Atkin (2003) Options for Screening for Colorectal Cancer, Scandinavian Journal of Gastroenterology, 38:237, 13-16, DOI: 10.1080/00855910310001421
[4] Shinji S, Yamada T, Matsuda A, Sonoda H, Ohta R, Iwai T, Takeda K, Yonaga K, Masuda Y, Yoshida H. Recent Advances in the Treatment of Colorectal Cancer: A Review. J Nippon Med Sch. 2022 Jun 28;89(3):246-254. doi: 10.1272/jnms.JNMS.2022_89-310. Epub 2022 Jan 25. PMID: 35082204.
[5] Johnson CM, Wei C, Ensor JE, Smolenski DJ, Amos CI, Levin B, Berry DA. Meta-analyses of colorectal cancer risk factors. Cancer Causes Control. 2013 Jun;24(6):1207-22. doi: 10.1007/s10552-013-0201-5. Epub 2013 Apr 6. PMID: 23563998; PMCID: PMC4161278.
